CASE REPORT
A 55-year-old male patient was referred from the ear, nose, and throat department of Chettinad Health City to the Oral Medicine and Radiology Department for a dental opinion. With a chief complaint of multiple eruptions in his face, scalp, mouth along with facial deviation present for 4 days. On probing more into the history, the patient revealed continuous, radiating pain to his right side of the face, ear, and oral cavity for the past 2 days and further reported experiencing low-grade fever accompanied with facial disfigurement. The patient gave a history of experiencing an episode of chickenpox during his childhood. The patient’s medical history revealed that he had diabetes with poorly controlled glycemic status for the past 5 years.
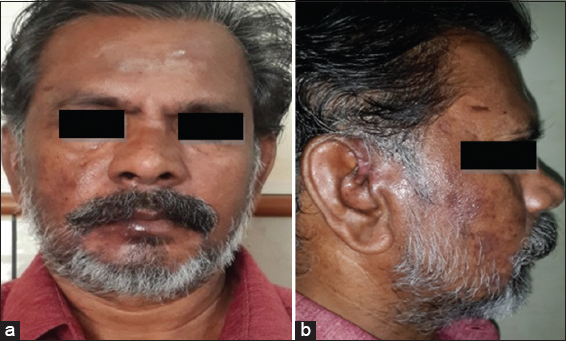
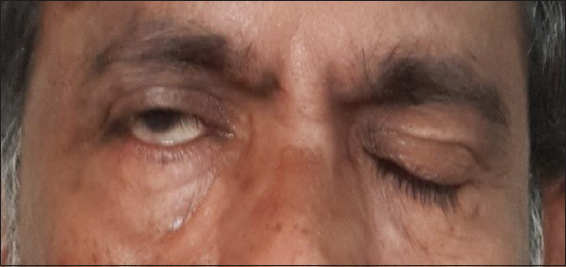
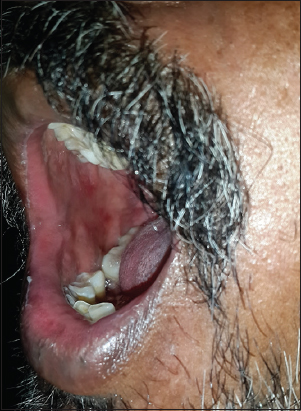
On extraoral examination, multiple vesicles were noted over the external auditory meatus, multiple macules with crustations over the right side of the scalp, face, zygoma further extended to the lower lip [Figure 1a and b]. There was the absence of wrinkles on the right forehead, the inability of the patient to close his right eye completely [Figure 2], and mild drooping of the right commissure of the lip. Intraoral examination revealed multiple vesicular eruptions with a clear fluid discharge on the right buccal mucosa [Figure 3]. Hence, the provisional diagnosis of RHS and differential diagnosis of Bells palsy, neurosarcoidosis, and Parry Romberg syndrome were given. Laboratory investigation with a hemogram, serum glucose levels, serum electrolytes, and a peripheral blood smear was done. Except for the increase in serum glucose level, other test results were within the normal limits. The patient was subjected to a Tzanck smear test, which revealed multinucleated giant cells, thus based on the above findings, a final diagnosis of RHS was derived. The patient was prescribed acyclovir 800 mg five times a day, Tablet acetaminophen 500 mg q6 h tablet prednisolone 20 mg od and vitamin supplement twice daily for 7 days and were asked to report of a review. The patient was told to rest and stay hydrated. After 2 months, during which the complete regression of lesions was noted, he returned for follow-up. Later, the patient was under physiotherapy and transcutaneous electrical nerve stimulation (TENS) therapy to regain muscular activity post-facial paralysis; the degree of facial paralysis was Grade III, using the House-Brackmann Scale [Table 1].
Figure 1. (a) Crustations were evident along the right side of zygoma further extended to the lower lip; (b) scalp and face involving tragus of ear
Figure 2. Inability to close eye completely
Figure 3. Intra oral vesicles seen in buccal mucosa
Table 1. House Brackmann Scale for grading facial palsy
| Grade | Function level | Symmetry at rest | Eyes | Mouth | Forehead |
|---|---|---|---|---|---|
| I | Normal | Normal | Normal | Normal | Normal |
| II | Mild | Normal | Easy and complete closure | Slightly asymmetrical | Reasonable function |
| III | Moderate | Normal | With effort complete closure | Slightly affected with effort | Slight to moderate movement |
| IV | Moderately severe | Normal | Incomplete closure | Asymmetrical with maximum effort | None |
| V | Severe | Asymmetry | Incomplete closure | Minimal movement | None |
| IV | Total paralysis |